Tuesday, October 12, 2010
the long-awaited ct
I'll not keep you in suspense. The CT went well. The infection is completely gone as far as they can tell. I have some inflammation around my sternum, but that has been showing up in CTs since the transplant and hasn't gotten any bigger. Also, it looks like the persistent-if-slight pneumothorax is all but gone. So, all good news.
Also had another lung function test, and the numbers were stable, improved just a tiny bit. The stomach is still an issue, and doesn't seem to be improving much despite a new med, so I'll just have to wait it out, I suppose.
That's about it. Back to the doc's in a month to make sure things are going smoothly, and I'll see where I go from there.
Thursday, September 23, 2010
goodbye, philly
now i'm back to a sort of waiting game. i've stopped all the antibiotics, but no one is totally convinced that the infection has been completely erased. so on october 12, i'll have one more CT scan to check everything out to be sure the infection has gone the way of the dodo. if it resurfaces by then, not sure what we're going to do, since the one antibiotic that kills it also knocks me on my ass and obliterates my kidneys. so here's hoping the infection is gone completely.
after the appointment, dad and i packed up the last of the philly apartment and turned in the keys. i wasn't too sad to say goodbye, frankly. it was a nice place and all, but it's been a rough few months and it's a lot more comfortable to be back in nj with the parents around while i re-rehab. the past few weeks negated a lot of the work i did to get back into game shape, so i'm practically starting from square one in terms of regaining my strength and putting back on the weight i lost (again) from this most recent ordeal.
so anyway, i'm back in nj for good. staying with the parents again, for now. still trying to get up and running.
Saturday, September 18, 2010
Hospital stay over, for now
As I said, I got admitted for acute renal failure that we all assumed was a result of the colistin I was on to combat the infection that I had surgically drained on my previous stay. So when I got here, they stopped all the antibiotics and started pumping me full of IV fluids in order to flush out my kidneys. Slowly but surely, my kidney function has been trending positively and is on the verge of being completely normalized. So that's good.
While they were waiting to see if the fluids were working, I had an ultrasound of my kidneys, to make sure there was not a physical problem with the kidneys that might be causing the renal failure. As expected, everything there was normal.
So into the next test. Since they had stopped the antibiotics, the doctors wanted to be sure that there was no infection growing where the abscess had been, so they ordered a CT of my chest and neck. Well the area where the abscess had been looked improved, but they saw something they didn't like around my aorta: either a hematoma or an infection. Either one was likely the result of the abscess surgery, but while a hematoma would not be a big deal and would heal on it's own, an infection would be a major problem, especially since the antibiotics needed to fight it had done a number on my kidneys. So, more testing to figure out if it was an infection. Normally, they would have ordered a CT with contrast, but they didn't think my kidneys could take the contrast in their current condition, so I was headed to nuclear medicine.
In nuclear medicine they did a tagged white blood cell scan. Basically, they took 50ml of blood from me, separated the white cells, and tagged them with radioactive material. Then they reinject the white cells, wait a few hours and scan my chest to see if the white cells cluster anywhere. The idea is, since white cells attack infections in the body, the radioactive white cells would head for any infected area and you'd see a cluster of white cells on the scan. So if the white cells clustered around the suspect area of my aorta, that would mean that the abnormality on the CT scan is in fact an infection. For once, I dodged the bullet. The WBC scan came back negative for infection. In fact, the white cells did not even cluster around the old abscess region, so presumably there is no remaining infection there. The conclusion is that the spot on my aorta is a hematoma and the spot around the old abscess is just some inflamed tissue.
So the plan now is to discharge me today, without any antibiotics to make sure my kidneys can heal all the way. And then I'll have a follow-up CT with contrast in a couple weeks to make sure everything is a-okay.
I'll be heading back to NJ and moving out of the Philly apartment. And hopefully things will go a bit more smoothly now.
Tuesday, September 14, 2010
back to the hospital, again
now to the bad news. had some blood work done today and then went in to see the dr h. it seems my kidney function is way high, as is my tac level, and i am in some sort of acute renal failure because of the combined toxicity of the tac and the colistin. so i'm headed back to the hospital as soon as a room opens up for me. the plan is to hydrate me with iv fluids, monitor the tac and creatinine levels and get them under control, make sure there is no permanent damage to my kidneys, and figure out a way to continue treatment for the previous infection at nontoxic levels.
Wednesday, September 8, 2010
Day 8: Discharge
it looks like the bacteria that made up the abscess was a new one to my body. it is still pseudomonas, but a different strain than was present in my lungs/body before the transplant. and no one has any idea where it came from. one theory was a esophageal tear, but there is no evidence of that. another was that the infection migrated from the left anastamosis when the stent was removed, but the location of the abscess makes that very unlikely. so i am left with a very drug-resistant bacteria, no real explanation as to how it got there, and no confirmation that the drugs i'm taking will kill it. we should know from the lab results if the bacteria is resistant to the colistin i am on in the next few days. but all this is a troubling development, as dr h put it.
so i am home, but i am looking at 6 weeks of IV and oral antibiotics. also i have a small rubber tube, a penrose drain, sticking out of my neck and secured with a safety pin. no joke. dad gets the pleasure of retracting it an inch every two days until it is all the way out. that should take a week or less. meanwhile the drugs and the hospital stay have left me kind of dizzy. not sure exactly what that's about, or if it's going away anytime soon.
in related news, today is three months and one day since the transplant. it's about the time i expected all the major recovery issue to be wrapping up. go figure.
Monday, September 6, 2010
Hospital Day 6
The surgery went fine and I now have a straw sized tube sticking out of my neck to continue to drain the fluid in the cavity where the abscess was. Swallowing is fine now, but I have some limited mobility in my neck because of the incision and the bandages. The incision is apparently two inches long. So I'll have another fantastic scar to show off.
Meanwhile, they are hitting me with a kitchen sink of antibiotics because they are still not sure what sort of bug was in the abscess. The sample they took has grown gram negative rods, but they are waiting for further growth in order to identify the specific species and subspecies of bacteria so that they can properly focus the antibiotics. They should know that by tomorrow or Wednesday. Tomorrow I will also have a CT to assess the situation
Mom, Dad, and KC have been hanging out at the hospital with me, but I'm not very good company.
That's about all I've got. Enjoy your Labor Day.
Friday, September 3, 2010
Dad's Hospital Update # 1
At this time he is in Recovery and I expect to be able to see him in an hour or so, then off to an inpatient bed somewhere. It looks like he will be in the hospital for a few days while they wait for lab results and to see what if any additional antibiotics are indicated.
That is all I know at the moment.
Justin
Hospital update
No surgery is without risks, of course, but one of the residents did describe this as "child's play" compared to the transplant. Though this surgery is complicated by my post-transplant immunosuppression. Not sure how long the surgery will all take, but it looks like I'll be in the hospital a few days recovering and I'll probably leave on more IV antibiotics. Hopefully everything goes smoothly.
Still no idea what caused the abscess, but they may be able to determine that based on what they see inside.
Thursday, September 2, 2010
Hospital holiday
If you've been keeping up, you can probably guess that the CT Wednesday morning did not go terribly well. They found some sort of abscess in my mediastinum that is excerting pressure on my esophagus and trachea, and displacing my esophagus slightly. Hence the swallowing problems ive been experiencing. The abscess seems to be a pocket of fluid, about 3x5 cm, though they cannot determine the nature of the fluid and are not sure if it is infectious. So the solution is to go in and drain the abscess and test the fluid to see what we are dealing with.
And that is where the fun begins. I'm on an interventional pulmonary service, and so far they've consulted with interventional radiology, cardiothoracic surgeons, and the ENT team. No one seems particularly excited to tackle the problem. CT Surgery is deferring because their procedure would be the most invasive. But ENT insists that the abscess is too far down and out of their specialty range. And IR doesn't think they can get at the abscess because it is blocked by lots of blood vessels and major arteries. So by default it looks like it's going to be cardiothoracic, though they are consulting with other ct surgeons to determine who should have a go and how best to attack the abscess.
So, having checked into the hospital yesterday around 4, ive been here 20 hours, seen about a dozen docs, and there is still no real plan. Basically I'm just sitting in my lovely hospital room with it's shitty tv waiting to hear back from cardiothoracic. They may schedule something for tomorrow or maybe not untill next week. If they push it back to next week, I will probably insist on going home for the weekend, but we shall see.
I'll keep you posted.
Tuesday, August 31, 2010
Overdue Medical Update
a couple weeks ago, i started experiencing this weird feeling in my throat, like something is lodged there and won't go down. so every time i swallowed, it was pretty uncomfortable. it got worse over the past week, so yesterday i underwent a barium swallow study: basically i drink a thick, chalky liquid in various standing and laying positions while they take pictures of my esophagus and upper g.i. area. the results were inconclusive in terms of the swallowing issue, but did show more acid reflux. so today dr. H upped my acid reflux med and ordered a throat CT w/ contrast (tomorrow a.m. -- yippee) to check for inflamed nodes or something of the sort that may be pushing on the esophagus from the outside.
meanwhile, the stomach issues have been coming and going. had some severe pain a few weeks ago, then it went away, then it came back, etc. so we are swapping out two of the g.i. meds (reglan and erythromycin) for domperidone, a med not approved in the US, but used extensively in canada (where dr H used to practice). this means i have to order it from some pharmacy in canada. just one more hassle. but hopefully it will solve the stomach issues.
of paramount importance, of course, are the lungs. i had a bronchoscopy this past friday. no rejection, no growth of fungus or bacteria, no major cleanup necessary. the only hiccup was that the left anastamosis (the one that had the stent for the dehiscence) healed very narrowly. so it took some forceful prodding to get the bronch scope in. the resulting inflammation and all the poking and prodding knocked me off my feet, so to speak, for a few days. but it looks like the airway may have opened up a bit, because my FEV1 (lung function) is up to its highest point, at 49%, a marked increase from testing three weeks ago. but as a result of the narrowing, unless the lung function drastically improves, they may need to put in a sort of balloon to widen the airway in november.
the other open issue has been my energy level, which has been particularly low the past couple weeks. this one seems to be a mystery. all the blood levels have come back normal and we can't seem to pinpoint the cause. i'm discontinuing one heart med that may be contributing to the problem, but otherwise it seems to be a wait-and-see sort of scenario. hoping that fixing the other problems will help fix this one.
that's about it. overall, i'm no tin bad shape. no major setbacks. just a few little ones that are being consistently uncooperative. so hopefully something will break in my favor. and hopefully the CT tomorrow will illuminate this swallowing issue. and with any luck the lung function numbers will start climbing regularly now.
Wednesday, August 18, 2010
nothin doin (america edition)
my bronch has been pushed back a week for scheduling reasons, but i went in yesterday for some bloodwork. i haven't heard back about any of the results, which means everything is a-okay.
after bloodwork, i decided to waste the day in high american fashion, so i spent a few hours driving and walking around valley forge. honestly, i spent less time thinking about the torturous winter months of 1777-8 than about things like "i wouldn't have been able to walk up this hill 3 months ago" or "i don't even care how far away i park anymore". a different sort of introspection than the founders intended, i'm sure.
to make it an even more american day, i proceeded to a mall. and not just any mall, but the vast, unwieldy megacampus of king of prussia mall. why did i do this, when i so obviously hate malls? i was looking for food. of course, i ended up parking on the complete opposite end from the food court, so i got plenty of exercise and wandered into plenty of stores for no apparent reason. in my travels i managed to acquire 1 sandwich with fries and coke, 1 crazy indie novel, 1 dirt-cheap pair of jeans, and 1 iced coffee.
and that was about it. some history. some selfish introspection. and some consumerism. pretty darn american.
Wednesday, August 11, 2010
(bi)weekly medical update
my lung function is no better or worse than it was 2 weeks ago. in a glass-half-full world, this is good news, because nothing is wrong and my lungs are already in better shape than they have been in 15 years. in my world, this is frustrating news, because i expect my lung function to improve beyond 46%, but it is constantly stagnating. dr. h. said the l-fn could improve for as long as 1 year before it levels off, or it could very well have already levelled off. the sound of his voice wasn't super-confident when he talked about my l-fn slowly increasing to 80%, but maybe i'm just projecting. anyway, only time will tell.
and apparently time is about the only medicine for my recent g.i. issues. i've been having some severe stomach pain in the evening, after dinner, for which there is nothing to be done but eat a little less and wait. that strategy made sense to me two months ago, but now it seems a little inadequate. i really thought i was done with the stomach issues, but they've resurfaced the past couple weeks.
there is good news, of course. news good enough that even i can't spin it negatively. blood sugars have been fine, so i am the rare case of a cf patient not developing diabetes post-transplant. rare as in less than 10%, as in only the second patient dr h has had in the past 5 years. so the plan is to still check it a few times a month, just so that i don't miss it developing at a later date (which could still happen), but otherwise i am free of that hassle for now.
dr h scheduled me for a bronch in two weeks (just to check everything out and be on the safe side). and otherwise just occasional blood work and less occasional chest xrays and office visits. so i'm just chillin in philly for the foreseeable future.
Tuesday, August 3, 2010
rehab is fin
in other medical news, since i've been ok for the last week, they finally pulled the picc line, so i am now completely unfettered. and blood work has been knocked down to once a week, doctors visits bi-weekly, and xrays every two or three weeks.
so, i will be coming up to nj for a long weekend on thursday. ill be in wayne till monday, so if you're around....
i think ill spend wednesday at the philadelphia museum of art. ill probably be able to make it all the way up the rocky steps, and then i can relax in front of some renoir.
Wednesday, July 28, 2010
weekly medical update
xray is improved. after 3 weeks of antibiotics and the stent, the pneumonia seem to be cleared up and the pneumothorax has gotten a tiny bit smaller. and i've stopped the iv antibiotics, thought the picc line is still in.
all my drug/vitamin levels are within range, though the tac level is at the low end, so may bump the tac back up to 2.0mg.
with the blood sugars totally under control, i can reduce the blood sugar checks (read: finger sticks) to twice a day, down from four times a day. if things stay stable over the next couple weeks, i can abandon the pseudo-diabetes blood-sugar-check behavior altogether.
my lung function was up to 49% (from 45%). good to see it moving up again. let's hope it stays moving in that direction.
and, the biggest news of all, next week will mark the end of rehab. just a few more sessions and i'm out of there. i will have completed the prescribed number of rehab sessions, and i've pretty much peaked in terms of how much they can exercise me in their little gym, so i will be released out into the world to fend for myself. which means i have to come up with some sort of self-motivated exercise routine.
that's about it on the medical front. i'm not due for another check in with the doctor for two weeks, so the weekly medical update may become a bi-weekly medical update. or it may just be totally irregular.
in nonmedical news, i am home alone, shockingly surviving on my own once again. i've officially begun the period of my renewed independence, and what was formerly my parents' bedroom is now officially the guest bedroom. (sorry, mom and dad. but thanks for being here when you were. you are still allowed to come visit.) i have slipped pretty easily back into my living alone routine; it's nice to know that it still comes easily after all this time.
i hope you all have a lovely wednesday.
Saturday, July 24, 2010
Friday Is Bronchday II
so this time, the bronchoscopy (#4 since transplant, in case you're counting) was supposed to be at 2:30. which sounds nice until you consider that the patient must fast starting at midnight the night before. 2:30 being what it is, i cheated slightly and took my morning meds with 6oz of black coffee. harmless.
so i planned to be at the hospital to check in around 12:30, though i had received no call the night before to confirm. well, at 11a, dad got a call at home from the interventional pulmonology folks to tell me that they had been expecting me at 10:30. so mom and i scrambled to get out the door, and i checked in about 11:20. good thing, too, because then i had to wait 3.5 hours until the procedure. (that brings my total for the week to 8.5 hours in hospital waiting rooms. [it could be worse, jim, i know.])
but in the end, the bronch went as well as could be. they removed the stent, and the dehiscence in the left anastomosis had healed well enough that they did not have to put another stent in. so good news that things are healing and good news that i wont have to undergo another bronch for 6 weeks or so, provided no more bumps in the road. while they were in there, they cleaned up a few secretions and whatnot, but nothing major. so the dehiscence is healed and the lungs look nice and clean.
good thing i shaved off the beard last weekend.
so on to the weekend: a little housewarming party at my cousin's this afternoon (and the house will be warm: heat index to 110 here in philly today), and then some long awaited visitors on sunday.
for now, it's back to my coffee.
Tuesday, July 20, 2010
weekly medical update
the good news is, the driving restriction has been lifted. in and of itself, this is maybe not huge. but it is the first step to resuming independence. and it's nice to take a step in that direction. it was also nice to actually drive my car for the first time in 6 weeks or so. it's just like riding a bike. and i didn't hit any cyclists on the way home from rehab.
the notgood news is, my lung function has plateaued again, i have another bronch scheduled this friday to swap the stent, and the IV antibiotics have been extended another week. so none of that is much fun.
the CT scan did show a decrease in the pneumonia and pseudomonas colonization, but the bronch last week seems to have rustled up some junk in my left lung, which is why they're playing it safe and extending the antibiotics. of course, if the bronch does that every time, i'm going to be stuck in an endless loop of IVs and bronchs. unlikely, of course. but i'll feel better when the lung function is climbing again and the bronchs are less than a regular occurrence.
also, they'll be taking another biopsy during this bronch to check for rejection. which is not standard procedure, so i'm wondering why in particular they made that decision.
anyway, dad is heading home tomorrow on the train, so i will be on my own -- for the first time in a long time -- until....thursday night. then mom comes back down because i need a ride to/from the bronch. but i guess 36 hours of independence is a nice test run.
Sunday, July 18, 2010
sans beard
playoff beards are supposed to bring you good luck and keep you on a hot streak. right now the only streak i'm on is one of unsatisfying bronch results. so yesterday i nixed the rehab beard, 'cause it aint doin' me any favors.
that is all.
Friday, July 16, 2010
Friday is Bronchday
we -- mom and I -- got to the hospital at 6am on the dot, sans morning coffee (fasting for bronch). well, mom had coffee. i had pills. through admission and gowned by 6.30a.
then we talked to the interventional pulmonologist, Dr G, and his fellow, whose name ive already forgotten, so we'll call him Dr NA. this bronch was to be a lot more involved than the last one, with the possibility of inserting a stent (if the dehiscence hasnt improved) and the possibility of having to do a rigid bronch (which involves inserting a stiff metal tube down the throat, into the airways, through which the Dr can use things like forceps and cameras and various tools that one should not normally have shoved down ones throat). either way, Dr G informed us that this was very likely the first of a long series of bronchs (news to me) over the course of the next few weeks or months until everything looked copacetic, at which time i could go back to having just the regularly scheduled bronchs through the transplant clinic (which is where the first one was, two weeks ago). since they were playing the whole procedure by ear, depending on what they found when they peeked inside, it could take an hour or 4 hours or anything in between.
and with that lovely news, i was rolled into the OR and pleasantly shoved into a drug-induced nap.
did i forget to mention the baby-faced medical student who got to hold the oxygen mask? i hope he didnt get to do anything else while i was passed out, because honestly he couldnt have been over 13. i refrained from all doogie howser jokes, though. arent you proud?
i spoke to Dr NA a couple times after they woke me up (procedure < 60min.) heres the deal: they put in a temporary stent; rigid bronch was not necessary; there was very little cleaning inside the lungs necessary.
the idea behind the stent is to promote the formation of tissue in the left anastomosis in order to solidify and widen the airway. in 2 weeks, theyll go in again, and take out this stent and replace it with another to further widen the airway. this will be done ad nauseum every two weeks until they are satisfied with the state of the airway. as far as i can tell, it might be done 2x or it might be done 20x. all depends on the healing.
as for the cleaning out, the fact that not much was necessary is the good news for the day. very little pseudomonas colonization and mucus clogging. im hoping this means the ivs can be stopped next week, but Dr NA could provide no guidance on this.
now i am home, finishing cup of cafe dos. no plans this weekend. it might be too hot to go outside, ever. we shall see.
Wednesday, July 14, 2010
Weekly medical update
Dr H is on vacation in Greece or someplace, so this week's appointment was just with B, my nurse practitioner.
Things seem to be moving in the right direction. My stomach issues are nearly entirely resolved. Potassium level is back to normal. Tac level is a little low, so we are upping the tac dose. Lung function is moving up again after a week-long plateau and is now at 45%.
The big questions will be answered on Friday when they do the bronchoscopy. Depending on what they see when they go in there, they may put a stent in the left anastomosis if the dehiscence is not healed/healing. The look of the bronch will also determine whether or not they continue the IV antibiotics beyond the initial two weeks. Obviously, I'm hoping for no stent and no more IVs.
In News of Christopher's Eventual Independence, the ban on driving will be lifted next week. This is the first step in kicking my parents out of the apartment they found me and resuming something close to independent life. Mom and Dad have been great, and I couldn't have done any of this without them, but I'm pretty eager to make my way back to life as normalish.
MT, my old neighbor, came down to visit last night. So I got a healthy dose of old Wayne. Oh, and cupcakes. Today DD is coming down, so I will be cheerfully entertained all day. And then back to rehab on Thursday. Bronch on Friday. What fun.
Sunday, July 11, 2010
Obligatory post
CN came to visit for the weekend and We spent lots of time watching the last two world cup games and walking around aimlessly and just generally doing lots of nothing.
Next week's schedule: blood work, rehab, xray on Monday; rehab and appointment with my NP on Tuesday; blood work, rehab, and xray on Thursday; and another bronchoscopy on Friday to see if the dehiscence has improved.
That is all. Have a lovely day.
Wednesday, July 7, 2010
monthiversary
[i suppose i am supposed to be reflective. or something. but i'm not. probably because i am still in the middle of it all, so i have very little energy to start looking back at this point. i'm not in hindsight 20/20 territory yet. so we'll leave that for another day in the (hopefully not-too-distant) future.]
to celebrate i refrained from any physical contact with any medical personnel and maintained a strict 1 mile dmz between myself and the hospital. though i did have to field about half a dozen medical-related phone calls. which was a little excessive.
but i did get some good news. the biopsy results from my bronch last week came back and there is NO rejection. which is a welcome relief, considering treating the rejection is counter intuitive to treating the dehiscence in the left anastomosis. also, my tac level has finally settled into the proper range, so i won't have to adjust the drug levels.
nice to get some good news after the past week.
tomorrow, it's back to rehab.
Tuesday, July 6, 2010
discharge (again) and weekly medical update (again)
today, however, was mostly antigood. i spent most of it sitting in my hospital room just waiting for the folks at the hospital to get their act together and get everything ready for discharge. by 10am, they had made the decision to discharge me, but i didn't actually leave the hospital until after 6pm. so it was kind of a long and frustrating day of very little progress.
which is kind of how the entire last week has been. instead of feeling a little better every day, i have stalled out and really don't feel any better than i did a week ago, and the test numbers and images confirm it. in the past week i've had about 6 chest xrays, a chest ct, and a bronchoscopy with a biopsy. the results of the biopsy still have not come back (the point of the biopsy is to see if there is any rejection, btw), but from all the rest they have determined:
1. the suture rupture in the left anastomosis is a major issue. with only the one bronch, we cannot tell if it has started to heal, so there will be another bronch likely in the next week. if things do not improve, they may have to insert a stent to promote some scar tissue. in the meantime, the prednisone has been lowered (which is good for the blood sugars, but bad for possible rejection) in order to help the healing process;
2. there is definitely pseudomonas present. can't tell for sure if it is new and active or an old colonization, so we are pumping me full of iv antibiotics (which i was sort of hoping to be rid of after transplant) and some nebulized antibiotics (another thing i was hoping id never see again: nebulizers);
3. the pneumothorax has not gotten worse, but it has not improved. if it gets any larger or starts to leak into other parts of the lung, they may have to put a chest tube in (another thing i thought i was rid of) to drain the pleural fluid.
in the meantime, i am home at least, on iv antibiotics and nebulizers and some extra oral meds for at least the next two weeks.
dr h summarized the situation as: a "significant step back/bump in the road", but one he expects me to fully recover from and move on from.
so that is that. i am mostly worn out, though i think it's more psychological than physical.
Monday, July 5, 2010
bells and the afternoon brought hours of playing rummy 500 with mom.
In the morning one of the residents informed me that there was fluid
in my lungs, filling the pneumothorax, and that my hemoglobin was
getting dangerously low. Turns out the hemoglobin was probably a lab
error (reran the test and number was ok) and after hours of fretting,
the attending informed me that fluid filling the pneumo was perfectly
normal, and everything was going as expected. The pneumo hadn't gotten
bigger so there was nothing to worry about.
Then, hours of the ongoing card game with mom. I forget who's winning.
I slept through the fireworks, sort of. Mom, dad, and Aunt E watched
them from the hallway with a bunch of other patients.
That's it. Usual blood work and chest xray planned today.
Sent from my iPhone
Saturday, July 3, 2010
Male nurse day
occassional male nurse: it's a nice change of pace. This guy was like
a toned down version of the case-of-the-Mondays waiter in Office
Space. Actually I kinda like the guy, but he said "these guys" way to
much. As in, You gotta take these guys first, referring to some pills.
And, I gotta hook this guy up, referring to an IV antibiotic. As I was
wheeled away for my kafkaesque trip to radiology for a chest xray he
actually said, I'll catch you on the flippy. No joke.
But he was a solid nurse. The newly annointed residents are another
story. I have them to thank for being underdosed on pain meds all
afternoon. Not that I'm in unendurable pain, but I could stand to be
in a bit less. Coaxing from me and badgering from the Dad eventually
got it resolved, but I'm not sure how many days of this I can tolerate.
Chest xray supposedly (read by first year resident) showed improvement
and, as the Dad continues to remind me, the fatigue issue seems
resolved, so I guess things are headed in the right direction.
Prednisone has been reduced to help fight infection, but the tac level
is still hard to pin down.
All my meds make me so shaky it's hard to type on the ol iPhone, so
until tomorrow.
Sent from my iPhone
Friday, July 2, 2010
From Founders 1476
It's 3 days since my recovery was deemed "all star". Well, that didn't
last long.
Today (after a great dinner Thursday night with S) I woke up feeling
pretty crappy: tired, weight lost, headache, wheezing, tight chest,
shaky. My bronchoscopy was sheduled for noon, so I figured I'd just
report the symptoms when I saw Dr H for the bronch. Some of it, no
doubt, could be attributed to fasting for the bronch.
Well the bronch didn't exactly go swimmingly. Much of it was clear,
but Dr H found a medial partial dehisence (a small pit without a true
hole and partial suture breakdown) in the left anastomosis. (you're
gonna have to look those up yourself. No links today.) Also confirmed
the pneumonia that came up on the CT scan. So I spent most of today
waiting in the outpatient bronch lab to be transferred to inpatient.
I'm here in my hospital room now, fresh from a convo with my three-
weeks-experience resident (oh the joys of the hospital in July)
waiting for a tray of cold hospital food.
The plan is to pump me full of some iv antibiotics and an profilactic
antifungal and hopefully send me home Tuesday.
We shall see.
Sent from my iPhone
Wednesday, June 30, 2010
weekly medical update -- all star edition
every tuesday, in addition to rehab, i have an appointment in the transplant clinic with Dr H and one of the Nurse Practitioners. this appointment is basically the full medical touchpoint, with issues ranging far and wide, long- and short-term, small and large, minor and major. and while medical news creeps into most every post on this blog (that is the point, isn't it?), i figured, since i'm getting a comprehensive update once a week, i'd give you one too. aren't i considerate?
this week, my regular nurse practitioner, B, was on inpatient duty, so dad and i met with N instead. we know her pretty well from emails during the listing and waiting process, and she's super smart and calm and prepared. we had a long talk with her and Dr H joined in after a while to add his doctorness to the equation. so here's the deal.
on my inability to sleep: basically, i haven't been sleeping too well. i'm up every day by 5:30 when the nightly percocet wears off. and i'm waking up about once every two hours (which is an improvement on the once-an-hour pre-transplant). part of it is pain, part of it is medication side effects. they don't want to prescribe any sleep aids, because i'm already on so many other meds that might interact, and because i've never before been on anything for sleep. so N's recommendation is to a) cut out caffeine after noon, b) relax in the afternoon but don't nap, and c) establish a consistent sleep routine with good sleep hygiene (which i think is a pretty awkward/funny phrase; makes me think more of bedwetting than anything else). i'm not really sure how i am supposed to simultaneously a) cut out caffeine; and b) not nap. coffee has always been a crutch for my inability to nap. as for establishing a sleep routine, it's harder than it sounds. for my whole life, my sleep routine has revolved around the 40-60 minutes of nebulizer treatments i had to do before and after bed. i don't have to do those anymore -- which is awesome, obvi -- but it leaves a big gap in my routine. tucking myself in these past couple weeks has felt awkward and unnatural to me. i have a feeling neither of these is going to counteract the drugs/pain issue, but i'll give it a try.
on my malfunctioning gut: the combination of a) cf digestive issues, b) the trauma of transplant, and c) the side effects of so many meds, has also resulted in some seriously uncomfortable gastroparesis. things just aren't moving properly through my gi tract. the result is some serious pain and discomfort after eating, and major gas issues (from both ends). (tmi? yea.) the problem of course is that i need to eat, and i need to really eat more than i normally would in order to get through the recovery process. which is, of course, in total conflict. i'm already on plenty of gi meds to try to counteract the side effects of the other meds, but they only do so much. the gastroparesis seems to be getting slowly better, but it is still mighty uncomfortable. (and the distended belly that comes with hides my previously perfect abs, which is disheartening.) but apparently, the only brilliant scientific resolution is: time. so i'm just supposed to keep doing what i'm doing and it will slowly resolve itself (hopefully) over the next few weeks.
on my swollen ankles/feet: my dame judy dench cankles returned this past weekend. i'm told it is not a major concern, as long as the swelling goes down every night, which it does. so i'll just keep an eye on it and try not to think of margaret thatcher.
on diabetes and blood sugar levels: not sure if i have mentioned this before, but i have added diabetes to my list of maladies. it was not unexpected. in fact, the incidence of diabetes in post-transplant cf patients is something close to 90%. it may go away as i am weened off some of the drugs, or it may be permanent. there's really no way to tell. but for now, i am cutting out lots of sugars, taking my blood-sugar levels three or four times a day, and dosing with insulin with every meal. it's a serious pain in the ass (or really, in the fingers) so hopefully it is transient. but it is under control for now, at least. i just have to keep the milkshakes to a minimum.
on tac levels: the major/most important drug i am on is an immunosuppresant called tacrolimus (or prograf). it is the main weapon in fighting organ rejection post-transplant. my blood levels are tightly monitored (twice a week) to keep the tac level at the proper range, and then the drug dosage is adjusted accordingly if things are not quite right. it often takes a few weeks for the tac levels to really settle into place, and mine have been fluctuating up and down from the low 5s to the high 19s. at this stage in the process, my tac is supposed to be between 8 and 12. monday's blood test put it at 5.2. so we have upped the tac dose back to 2.0mg. more blood will be drawn thursday to see how that's going.
on prednisone: in other dosage adjustment news, the weening off the prednisone has begun. prednisone is use post-transplant to help fight infections. it's also used to fight rejection, should that occur (it hasn't yet). it is one of the drugs that is a) screwing with my sleep; and b) causing the glucose/diabetes issues. so it's a good thing to start dosing down. Dr H dropped it from 30mg to 25.
and now on to the lungs, the part i know you've all been waiting for.
on my lung function: the primary test used to monitor my lung function is a pulmonary function test (pft) called a spirometry. it basically measures how much air i take in and push out. from that test, the benchmark number used to gauge my lung function is called the FEV1 (forced expiratory volume in 1 second). basically, it is a measure of how much air i can blow out in the 1st second of exhaling. pre-transplant, my fev1 was about 22% of normal/healthy/predicted. yesterday it was 41%. that is only a slight improvement on the 38% from last week, but it is higher than it has been since high school, and it is moving in the right direction. my FVC (forced vital capacity), the other major benchmark, measures the amount of air i blow out in the full exhale. that number is climbing at a much slower rate (and is actually still lower than pre-transplant), but this is to be expected. so all this is good news, droogies.
on my chest CT: last week, my chest xray showed two small pneumothorax. this means there were two pockets of air in my chest cavity where my lung should be. it's often caused by a partially collapsed lung. in this case, the pneumothorax is the result of a slight mis-sizing of the donor lungs. (it wasn't an error, it's just the reality of the situation that no two people are shaped alike.) basically, the lungs didn't quite fill my chest cavity, so there are some air pockets in the spaces. this should resolve itself over time, as the lungs expand, but we have to keep an eye on it to make sure it doesn't get worse for whatever reason. to that end, last week i had a chest CT done to rule out any major issues. the chest ct showed that a) the pneumothorax is very small and not a major problem, and not getting worse; b) the sternum is healing/fusing nicely and smoothly; but c) there seems to be a slight infiltration of pneumonia in the lungs. Dr H has decided not to overtreat the pneumonia since i am not showing any symptoms, but he has moved up the 6-week bronchoscopy to this week (which will be about 4 weeks) just to be on the safe side (and because he's going on vacation soon). so the bronch is scheduled for friday, which sucks something awful because i had some much anticipated visitors planned, and because i may miss the end of the netherlands-brazil quarterfinal. (go orange!) they'll be taking a biopsy to check for rejection and assessing the pneumonia issue. it should be fun.
a further note on the chest CT: over the years, i have seen dozens of my chest xrays, but i'd never really looked at one of my chest CTs. a few months ago, A, a med student friend of mine, showed me examples of a ct of lungs with bronchiectasis (present in CF, it is the enlarging/inflammation of the large airways). she also showed me a healthy lung CT (where the large airways -- those enlarged/inflamed circles -- are not visible). the difference, you'll noticed, is pretty marked. i had much the same reaction to that juxtaposition as i had when i saw the pictures of my explanted lungs: how did they work at all? yesterday, my ct looked like the healthy lungs. and to see the clean, healthy ct was sort of exhilarating, just like seeing the clean xray not long after transplant. it's mind-boggling to think what was there before.
my regular NP, B, stopped in to say hi and pulled out the final stitch from the chest tube holes. so all the stitches are out and i'm left with just scars and scabs. (and some staples in my chest, but you can't see those with the naked eye.)
overall , the visit went well. to give you a sense of the big picture, i'll tell you what N told me. when i asked her how i am doing in terms of the overall progress of my recovery she said, "you are an all star."
i refrained from agreeing with her out loud. you know, because i'm modest.
thanks to everybody at audible who sent a note with the care package. they took me quite some time to read through, which is a very good thing on so many levels. i look forward to seeing you all soon. no, really, i do.
perc dreams update: i've noticed that i've been getting beat up or shot in a large percentage of my dreams, especially toward morning (ie, when the nightly perc is wearing off). i'm wondering if this is my brain trying to explain why i feel like i "got hit by a bus" (which is a phrase every one at upenn uses to describe how your body feels post-transplant). that's not helping my sleep either.
Sunday, June 27, 2010
a good weekend
friday was visitor-free so i took the opportunity to shave off the transplant beard, which looked like this:
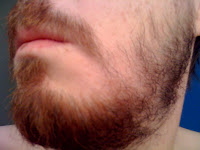
 combined with my pre-transplant laziness, it had been growing for about 7 weeks. now, it is gone. it was never quite wayne rooney's unkempt hobo beard, but it was getting a little out of hand. and i swear my chin changed shapes while hidden behind it.
combined with my pre-transplant laziness, it had been growing for about 7 weeks. now, it is gone. it was never quite wayne rooney's unkempt hobo beard, but it was getting a little out of hand. and i swear my chin changed shapes while hidden behind it.saturday brought with it a visit from 6 friends and my cousin. they came bearing gifts, as though i were jesus. even without the beard. so i got pizza (from nj), bagels (that smelled like home), pie (that was totally worth cheating on the diabetes for), and chocolate mousse cake (sugar free, but surprisingly good). unfortunately, they also brought bad luck, and the us fell to ghana 2-1 on some missed opportunities and ghastly defensive lapses. i hope you never play another game for the national team, ricardo clark. long live benny feilhaber.
lucky for me, all my friends were there to mitigate the misery of defeat. i was reminded how much it hurts to laugh a lot after major surgery. but, of course, it was worth it, and great to feel like things were semi-normal, even if i was in bed by 9 o'clock.
today i got a visit from two college friends. once again, we did very little but talk and watch soccer. and find out that most of the restaurants around me are closed for lunch on sundays. this would, of course, never have happened in dc where the restaurants are always open for sunday brunch. and once again im ready for bed mighty early, but pleased to be exhausted for good reasons.
mom has been here all weekend and made a lovely dinner this evening. she and dad will swap philly and nj tomorrow afternoon.
rehab tomorrow. then more rehab tuesday.
with the u.s. eliminated, ill be cheering for the netherlands. you should, too.
best percocet-induced dream last night: me as a guest on a late night talk show hosted by jack white, discussing jonah hill's new hiphop album, which was produced by jack white. oh, perc.
Friday, June 25, 2010
one week of rehab down
breathing continues to improve every day. im still working out in my head how to exactly describe the difference in feeling. it doesnt feel quite as "foreign" as it did at the outset, but it doesnt jive with my feeling of "normal" either. for the most part im feeling stronger every day, but by about 3 oclock every day i am pretty exhausted. and after dinner, due to various stomach/bowel issues, i usually feel kind of miserable. i need to eat smaller dinners.
thursday was the third and final day of the first week of rehab. the deceptively and demoralizingly simple rehab is every monday, tuesday, and thursday morning for two hours. thursday went something like this:
1. walk for 30 minutes at varied speeds averaging 2 mph; (time will be increased gradually to 45 min; then speed is increased)
2. take these pink 3-lb dumb bells and do really simple arm and chest building exercises, 2 sets of 10 for each arm; (weights will be gradually increased, i suppose, but because of the sternum cut, i am not supposed to lift anything over 5 pounds for a few weeks)
3. strap these 3-lb weights to your legs and do half a dozen different leg lifts and step exercises, 2 sets of 10 for each leg.
i couldnt help but think back to high school gym's weight training class as i concentrated on the reps. that was probably the last time i actually worked out in a gym.
despite the simplicity and the light weights, my legs are sore and my feet are starting to swell again. im not looking forward to tuesday's rehab, which will come without any luxurious days off beforehand.
mom i s back in town for the weekend. today we went to the reading terminal market and picked up lots of local, fresh food, and some much needed and delicious coffee and coffee beans at old city coffee (thanks for the rec, kowit). mom and dad are cooking up the tuna and scallops now. which will make the smaller dinners thing difficult. again.
of course, i totally forgot about the crowd restriction while at reading terminal. because of all the immunosuppressants, i am not supposed to be around crowds, especially indoors, for a few weeks. we tried to go before the lunch rush hour, but took longer than planned. dad managed to avoid freaking out about it though, which was nice. and we got out before it got too too crazy. death by the common cold averted. for now.
in more important news: go USA! i hope you all watched the US v Algeria game on wednesday. it was pretty intense. tomorrow i will be plopped in front of the tv (sadly must avoid the crazy soccer bars, thanks to aforementioned crowd restriction) with a whole gaggle of friends. dr. h cleared me to consume a beer or two in celebration if the US advanced out of the group stage (yes, i asked this specific question at my appointment on tuesday), though i'm not sure ill take myself up on the offer. we shall see.
tomorrow: official transplant beard pictures before i shave it off to begin the rehab beard.
down with ghana.
Monday, June 21, 2010
1st day of rehab
the first day of rehab is basically just to get some baseline numbers to work off of, so it wasnt too strenuous. and my baseline turned out to be a bit higher than they expected, which means im doing better than is typical 2 weeks out.
my goal is to get myself into running shape. this is kind of a big deal considering a) i am the slowest walker this side of 90 years of age; b) i am historically physically lazy; c) my peak, strenuous, tryinng my hardest walking speed is apparently 2.64 mph; and d) i have not run (sober) for anything in over 8 years. the last time i actually ran was in the spring of 2002. i was in galway. i was about 50 yards from a bus that i was about to miss -- a very infrequent bus, this being ireland -- and i ran to catch it, so that i would not miss the train to dublin. well, i caught the bus, spent the whole ride to the train station catching my breath, and got to the train 2 minutes before departure time. but -- remember, i'm in ireland -- the train proceeded to sit at the station for 45 minutes for no apparent reason. as it pulled out, so late that i couldve skipped the bus and just walked all the way to the station, i resolved never to run for any reason ever again.
so today i went to buy running shoes. (i tried to do this sunday, but ran into some availability problems.) it is a purchase i hae been looking forward to for many months. and i am now the owner of a shiny new pair of aasics. the first pair of running shoes ive bought since the summer of 1999. ill be breaking them in tomorrow at rehab day 2.
the trouble now will be to not overdue it and hurt myself. eventually, my competitive nature is gonna kick in. i imagine itll be like the opening scene of that episode of house when house's leg is tempoprarily healed. he runs 8 miles to work and arrives dripping in sweat. so im gonna try to avoid that. at least for now.
in other news, the beard is coming off. as soon as my razor and brush arrive from nj. off with the transplant beard, on with the rehab beard.
i wonder what it will be like when im no longer a lazy gimp....
Sunday, June 20, 2010
explanted lung pics
Day 14
Christopher is HOME, Of course “home” is now his apartment in Philly, but he is out of the hospital! He had his first home-cooked meal last night since the transplant. He likes his new digs, and complimented his dad on his efforts to find this place. All the important comforts of home including his cappuccino maker and coffee grinder. Chris even ventured out on his own least evening on foot, checking out his new surroundings, finding an ice cream shop, a breakfast place, an “interesting looking” restaurant, and the park. Apparently the walk went well though a few rest stops were included. Walking is good not only for lung exercise, but also to get away by himself. So now he can get settled in a new routine, getting in shape and getting his new lungs adjusted to their new occupant.
Pulmonary rehab starts tomorrow. It’s quite novel thinking about not including aerosol machines and IV medications into his daily schedule. And to not hear him cough and gag in the morning. Thank you to the donor, the transplant team, the nurses, and all the prayers from family and friends.
Just to put things into perspective, Chris gave me the okay to post a picture of his “old” lungs. He volunteered in a research project to donate his old lungs for research and asked that they send him photos of the explanted lungs. So these are the lungs that he was functioning with prior to June 7, 2010:
--Dana (aka Mom)
Saturday, June 19, 2010
"home"
with my hijacking, the following things will now be true:
1. updates will likely be LESS FREQUENT. frankly, if things go properly, there shouldnt be a lot happening, which is good, because there will be less crap to bore you with. and frankly, im not nearly as diligent as mom, so things will slip.
2. you can now expect regular injections of SARCASM (and insulin).
3. TYPOS will abound.
4. the blog will be FUNNIER. obvi.
5. you will get TIRED of me. unfortunately, if you signed up for email updates, youre gonna have to figure out how to unsubscribe by yourself. cause i dont care.
6. entries will probably be LONGER. because i am verbose. and terribly lonely (see #2).
as you know, i was discharged this morning. i am now "home" at the new apartment across the river from the hospital. pretty sweet digs, really. dad far exceeded my expectations. i guess i underestimate him sometimes. post-transplant requires that i have someone around all the time, so dad and i will be living the bachelor life (except when mom comes to town). he is out now stocking up on whiskey, beer, pizza, potato chips, and cigars. and tonight they are installing the stripper poll in the living room. ahh, the bachelor life. sorry, mom.
lungs are good, though they still feel sort of foreign. i dont know how else to describe it. i have to sort of relearn to breathe, in a way. but everything seems to be healing properly, as far as anyone has told me. but the new medication routine will take some getting used to.
today's big decision will be about my playoff beard. whether to a) shave off my transplant beard and start afresh sunday with my rehab beard; or b) keep the transplant beard through rehab as one long playoff beard. its getting itchy, so im leaning towards shaving. either way, i feel it is an important symbolic gesture to overgrow my facial hair like a superstitious atthlete until this is all over. we'll just have to wait and see if symbolism is more important than looking like a crazy irish hobo.
lastly, thanks to everyone who sent cards, emails, texts, comments, etc. it was overwhelmingly helpful to know that so many people were following along and pulling for me. (that is the first and last sentimental thing i will say on this blog. its just not how i roll. but it all really did help.) the staff was pretty impressed with my massive mail haul. and y'all know how i llike to impress strangers. you guys are the best.
Day 13 10:41am
A new segment of his journey has just begun...
Day 12
Actually, it is now Day 13.
Day 12 started out with some scary moments: Chris experienced 2 episodes of pretty severe tachycardia (that means, increased heart rate), the second episode more severe than the first. Scary for Chris and mom, but apparently it is not uncommon after such major surgery (what “major surgery”?, Chris asked—haha) when there has been manipulation of the heart, and much of the circuitry has been rewired. So a bunch of IV drugs and he was again concentrating on the world cup. Priorities—and diversion!
Justin, Chris, and I had our “Medications Discussion” with the transplant nurse, who very patiently and efficiently explained the purpose and dosing off each of the meds. There are actually 24.
The pneumothorax of Day 11 had resolved by mid-afternoon and his last chest tube was removed. He “celebrated” by taking a brisk stroll around the 10th floor unassisted and unattended (by a nurse), with an entourage of his 2 cousins and mom.
And the plan is for him to be discharged this morning.
--Dana
Dana O. Doheny, MS, CGC
Genetic Counselor, Research Coordinator
Mount Sinai School of Medicine
Department of Genetics & Genomic Sciences
1425 Madison Avenue, 14-75A
New York, NY 10029
212-659-6779 (O)
212-659-6780 (F)
866-322-7968 (toll-free)
